新しい研究は、骨髄移植後の成功したHIV寛解のXNUMX番目のケースを示しています
毎年少なくとも35万人がHIV関連の原因で亡くなり、約XNUMX万人が HIV。 HIV-1(ヒト免疫不全ウイルス)は、世界中のHIV感染の大部分の原因であり、HIVに感染した体液との直接接触によって感染します。 ウイルスは、免疫系の重要な感染と戦う細胞を攻撃して殺します。 HIVの治療法はありません。 現在、HIVは、HIVを抑制する能力のある薬を使用してのみ治療することができます ウイルス. These drugs have to be taken life long and it is challenging plus a cost burden on the health system especially in low-and-middle-income countries. Only 59 percent of patients of HIV worldwide are receiving Antiretroviral therapy (ARV) and HIV virus is fast becoming resistant from many known drugs which itself is a major concern.
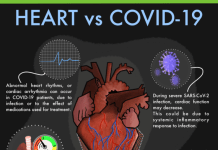
骨髄移植 (BMT) is a treatment used for leukemia, myeloma, lymphoma etc. Bone marrow, the soft tissue inside bones, makes blood-forming cells including the infection fighting white blood cells. A bone marrow transplant replaces unhealthy marrow with a healthy one. In the first case of successful HIV remission, an HIV-infected individual called ‘Berlin Patient’ who later revealed his name received a bone marrow transplant a decade ago when he was targeted to treat acute leukemia. He received two transplants along with total body irradiation which led to long-term HIV 寛解。
で公開された新しい研究では 自然 led by UCL and Imperial College London, the only second person has been shown to experience sustained remission from HIV-1 after a bone marrow transplant and stoppage of treatment. The anonymous adult male patient from UK was diagnosed with HIV infection in 2003 and was on antiretroviral therapy treatment since 2012. He was subsequently diagnosed with Hodgkin’s Lymphoma in the same year and he underwent chemotherapy. In 2016, he was given stem cell transplant from a donor who carried a genetic mutation which prevents expression of a most commonly used HIV receptor protein called CCR5. Such a donor is resistant to HIV-1 strain of the virus which specifically uses CCR5 receptor and thus the virus now cannot enter host cells. Since chemotherapy kills cells which are dividing, HIV could be targeted. From this understanding if one’s immune cells are replaced by cells which do not have CCR5 receptor, HIV can be prevented from rebounding after the treatment.
移植は、レシピエントの免疫細胞がドナーの免疫細胞によって攻撃される移植で一般的な軽度の合併症のような軽微な副作用で実施されました。 抗レトロウイルス治療は、HIV-16の寛解を評価するために治療を中止する決定を下す前に、移植後1か月間継続されました。 この後、患者のウイルス量は検出されないままでした。 患者の免疫細胞が重要なCCR18受容体を産生できなかったため、抗レトロウイルス療法が中断された後、患者は5か月後に寛解を維持しました。 この合計期間は、移植後35か月に相当します。
This is a second case of a patient exhibiting sustained remission of HIV-1 following a bone marrow transplant. One important difference in this second patient being that ‘Berlin Patient’ had received two transplants along with total body irradiation while this UK patient received only a single transplant and underwent less aggressive and lesser toxic approach of chemotherapy. Mild complications of similar nature were seen in both patients i.e. graft versus host disease. Achieving success in two different patients points towards developing strategies based on preventing CCR5 expression which might even cure HIV.
Authors state that they are monitoring the patient’s condition and cannot say with affirmation yet if he has been cured of HIV. This may not be a generalized appropriate treatment for HIV because of adverse effects and toxicity of chemotherapy. Also, bone-marrow transplants are expensive and carry risks. Nevertheless, it is a better approach with reduced intensity conditioning and no irradiation. Research could also focus on knocking out the CCR5 receptor using gene therapy in people with HIV.
***
{引用元のリストにある以下のDOIリンクをクリックすると、元の研究論文を読むことができます}
ソース
1. Gupta RK etal。 2019.CCR1Δ5/Δ32造血幹細胞移植後のHIV-32寛解。 自然。 http://dx.doi.org/10.1038/s41586-019-1027-4
2.HütterG。etal。 2009年。CCR5Delta32/ Delta32幹細胞移植によるHIVの長期管理。 N Engl JMed。 360。 https://doi.org/10.1056/NEJMoa0802905
3.ブラウンTR2015。私はベルリンの患者です:個人的な反省」、エイズ研究およびヒトレトロウイルス。 31(1)。 https://doi.org/10.1089/aid.2014.0224